In Part one, we discussed what DEFINITELY doesn’t work for Plantar Heel Pain (PHP). Then we looked at what MIGHT work based on present research. NOW, IT IS TIME TO LOOK AT THE EVIDENCE FOR WHAT ACTUALLY DOES WORK FOR PHP!
Weight loss
In a systematic review by Butterworth et al focusing on the relationship between body mass index and foot disorders, 12 of the 25 articles in their search results were related to chronic plantar heel pain conditions. These authors reported a strong association between greater body mass index and chronic plantar heel pain in nonathletic populations. Limited, weak evidence showed some change in pain following weight loss.

Obesity and pronated foot posture are associated with plantar fasciitis and may be risk factors for the development of the condition (Irving,D.B., et al, 2007). Wearing et al (2007) looked at arch shape and mechanics and found neither abnormal shape nor movement of the arch are associated with chronic plantar fasciitis, however, arch mechanics may influence the severity of plantar fasciitis, once the condition is present.
One of the difficulties with prescribing weight loss to a symptomatic PHP population is that exercise is often fundamental to this process, and maintaining a meaningful exercise routine with PHP can obviously be problematic.
Taping
A recent study has established a clinical prediction rule to identify patients with plantar heel pain likely to benefit from biomechanical orthotic intervention. In some ways, this is a bit of a game changer because, for the first time, it identifies a treatment path with an increased likelihood of success

Preliminary evidence suggests that anti-pronation tape has a neurophysiological effect as it alters the activity of several muscles of the leg during dynamic tasks such as walking or running. Taping may stimulate the sensory receptors through the surface contact or stretch of the skin to modulate the sensory input to the central nervous system.
Multiple anti-pronation taping methods have been proposed in previous studies, including low-Dye taping, augmented low-Dye taping, high-Dye taping and calcaneal taping.
Despite the results of two systematic reviews providing evidence for anti-pronation taping in decreasing the intensity of first-step pain, the effects of taping on improving function and decreasing disability are inconclusive.
Clinicians should use anti-pronation taping for immediate (up to 3 weeks) pain reduction and improved function for individuals with PHP.
Orthoses
The biggest concern relating to the use of orthoses in the treatment of PHP is not with regards their efficacy but with the design and degree or correction.

There is overwhelming evidence orthoses, both prefab and custom, are very effective as a first strike treatment for PHP.
The issue with the literature is that the designs are often inappropriate because they do not define the dosage of the intervention, nor the method of construction.
Putting that aside, let’s take a look at what we have.
This recent RCT concluded:
- Foot orthoses may be used for the prevention of common lower limb injuries in defence personnel.
- A reduction in common lower limb injuries can provide benefits for physically active individuals.
- Prefabricated foot orthoses provide individuals and employers with a relatively cost-effective intervention for the prevention of injury.
In many cases, the supposed “custom-built” orthoses all have identical posting and manufacturing processes applied, without regard to the differences between subjects.
The Cochrane review by Hawke et al found the following results regarding individuals diagnosed with plantar fasciitis:
“custom foot orthoses were more effective than sham orthoses in improving function, but not for reducing pain after 3 and 12 months; custom foot orthoses were not more effective than non-custom foot orthoses in reducing pain or improving function after 8 to 12 weeks or 12 months”
Ferber and Benson studied healthy individuals and found that plantar fascia strain was reduced by 34% when walking in either the moulded or non-moulded semi-custom foot orthoses.
The recommendation based on this study APTA heel pain guide 2014 JOSPT.pdf is as follows:
“Clinicians should use foot orthoses, either prefabricated or custom fabricated/fitted, to support the medial longitudinal arch and cushion the heel in individuals with heel pain/plantar fasciitis to reduce pain and improve function for short- (2 weeks) to long-term (1 year) periods, especially in those individuals who respond positively to anti pronation taping techniques”
This fits in nicely with the core clinical approach we use where accurate quantitative measurements are performed to determine an exact degree of prescription.
Surgery
Here is an example of the quality of research in this area. This study, states with some authority (but zero cross-referencing)
Conservative methods can provide a satisfactory outcome in up to 90% in the treatment of chronic heel pain. Resistant cases can be managed by a local injection of PRP; surgical management should be reserved for patients who do not respond to PRP injection
Well, no, because as we learned in the last Blog PRP does not work, so why would we benchmark that?
There are several techniques reported in the literature, however, one of the most promising appears to be radio frequency ablation of the medial Calcaneal nerve. This study provides a balanced view on the technique, stating:
“For patients with refractory plantar heel pain, ultrasound-guided denervation of the MCN can potentially improve symptoms, although efficacy needs assessing in comparative studies. Clinical Relevance: Ultrasound-guided denervation of the MCN provides a further management option for patients with refractory plantar fasciitis.”
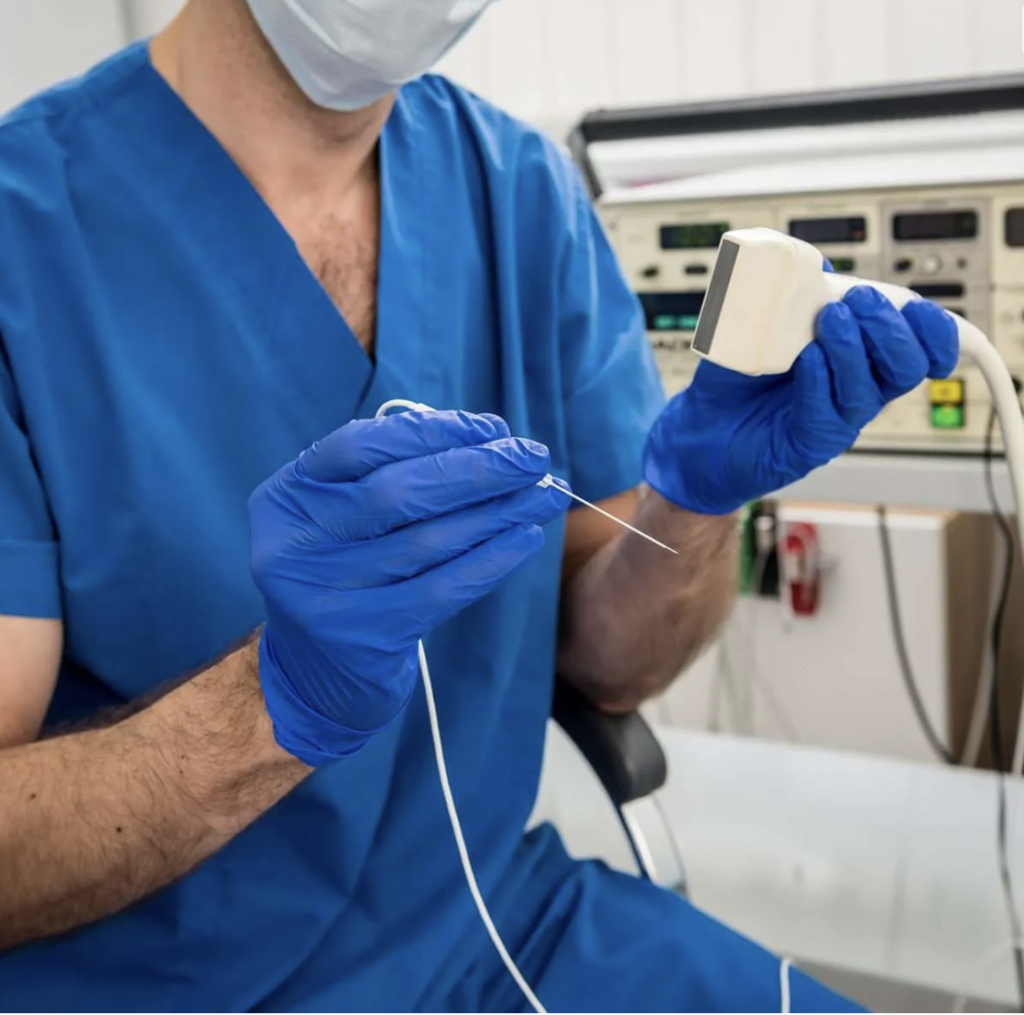
So, it is an option but unfortunately not widely available in Ontario.
By far the most common surgical procedure for the treatment of chronic PHP is endoscopic (minimal incision) plantar fascial release.
This study perhaps reflects the flavour of the results in the literature and interestingly folds this back into the likelihood of success based on Body Mass Index. Plainly stated below a certain BMI your chances of a favourable outcome are higher!
Surgery does appear to be a viable option with potentially good results, but only after all avenues of conservative management have been exhausted.
Right at the start of this little adventure, we identified that the single most important intervention for the management of PHP was weight loss. However, I purposely left its equally important cousin until right at the end.
Of equal importance is patient education, for without this, goal setting, and strict adherence, a favourable outcome with PHP is very unlikely. The education must cover all aspects, including the likely cause, best treatment options and especially the likely outcomes, and this education must be individualized.
So, this brings us to the end of our little summary of what does not work, might work, and does work for PHP. The purpose of this series was to better inform you, thus ensuring that the treatment regime recommended for your PHP recovery covers all options and is revised depending on your recovery progress.
Once again most of the hard work in researching/reviewing these treatments was done by Simon Bartold a world-renowned Australian podiatrist with impeccable credentials, a scathing sense of humour and an acute eye for detail in clinical research. His delightful paper on this subject was originally intended to challenge clinicians to analyze why they treat heel pain the way they do and make future choices more outcome-based.

If you have enjoyed our past blogs and videos, then like and subscribe to our Facebook or Instagram feeds. We will be updating them with a steady stream of new educational and informative subjects. If you have any subjects you would like us to write about then please send suggestions. We are easy to get hold of through any of our social media outlets or directly through our website @ www.podiatryassociates.ca




